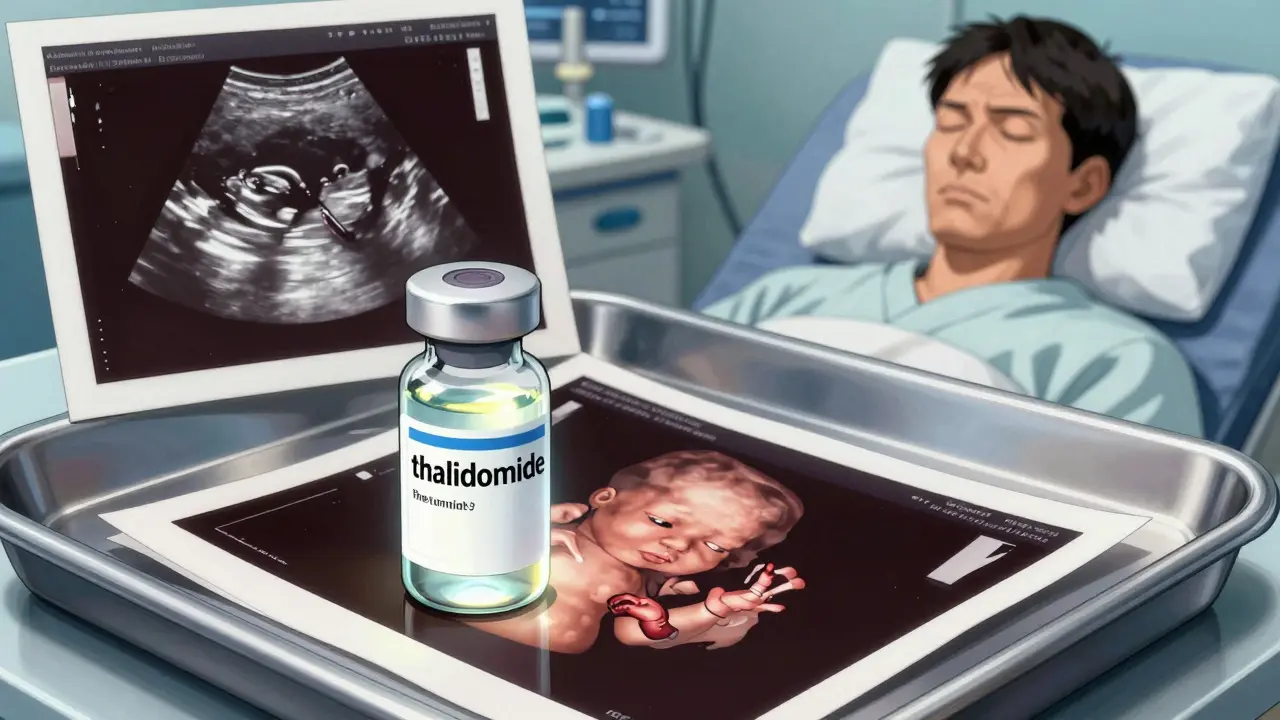
On a cold December night in 1956, a baby was born in Germany with arms and legs that looked like flippers. No one knew why. The parents didn’t understand. The doctors didn’t have answers. That baby was one of the first, but not the last. Within five years, thousands more would follow - children born without limbs, with missing eyes, damaged hearts, or internal organs that never formed. All of them had one thing in common: their mothers had taken a pill meant to calm nausea during pregnancy. That pill was thalidomide, a synthetic drug developed in 1954 by a German pharmaceutical company as a safe sedative and anti-nausea treatment for pregnant women.
How a ‘Safe’ Drug Became a Disaster
Thalidomide wasn’t some wild experiment. It was sold over the counter in more than 40 countries. Pharmacies stocked it. Doctors prescribed it. Mothers took it because they were told it was harmless. It was marketed as a miracle for morning sickness, insomnia, and even anxiety. No one thought to test it on pregnant animals. No one thought to ask: What happens to the baby? The answer came too late.
The drug’s teratogenic effects - meaning it could disrupt fetal development - only appeared during a narrow window: between 34 and 49 days after the last menstrual period. That’s roughly weeks 5 through 7 of pregnancy. Most women didn’t even know they were pregnant then. By the time they did, the damage was already done. A single dose could be enough. The effects weren’t random. They were precise: phocomelia (severely shortened limbs), facial paralysis, deafness, heart defects, and missing internal organs like the gallbladder or appendix. About 40% of affected babies died within their first year.
Two doctors independently connected the dots. In Germany, Widukind Lenz, a pediatrician, noticed a spike in birth defects and traced them back to thalidomide prescriptions. Halfway around the world, in Australia, William McBride, a young obstetrician, published a letter in The Lancet in June 1961 linking the drug to deformities. Within months, the drug was pulled from shelves. Germany removed it on November 27, 1961. The UK followed on December 2. But in the U.S., it never made it to market.
The Woman Who Stopped the Tragedy
In the United States, the FDA had received the application from Richardson-Merrell, the company trying to bring thalidomide to American pharmacies. The review fell to Frances Oldham Kelsey, a medical officer with a sharp eye for incomplete data. She refused to approve it. Not because she was skeptical of the drug’s benefits - she knew it helped with nausea. But she saw the lack of safety data, especially for pregnancy. She asked for more studies. The company pressured her. They called. They wrote. They threatened. She held firm. Her refusal, backed by scientific rigor, prevented what could have been a U.S. catastrophe. Kelsey became a national hero. And her actions changed everything.
How the World Changed After Thalidomide
Before 1961, drug companies didn’t need to prove safety or effectiveness. They just needed to say it worked. After the tragedy, the U.S. Congress passed the Kefauver-Harris Amendments in 1962. For the first time, pharmaceutical companies had to prove their drugs were both safe and effective before they could be sold. They had to disclose side effects. They had to conduct clinical trials. And they had to test for teratogenicity - especially if the drug could be taken by women of childbearing age.
Europe followed. The UK created the Committee on the Safety of Medicines in 1963. Other countries built similar watchdogs. Today, every new drug undergoes rigorous testing for fetal risk. Pregnancy categories (A, B, C, D, X) were developed based on this legacy. Even today, if a drug is labeled Category X, it means the risk to the fetus clearly outweighs any benefit - and it’s contraindicated in pregnancy.

Thalidomide’s Dark Comeback
Here’s the twist: thalidomide didn’t disappear. It came back.
In 1964, a doctor named Jacob Sheskin was treating a leprosy patient with severe skin lesions. He gave the man thalidomide - partly out of desperation, partly because it was still available in small quantities. The lesions vanished overnight. That was the first sign that thalidomide had powers beyond calming nerves. Later, researchers found it blocked the growth of new blood vessels - a process called angiogenesis. Tumors need blood vessels to grow. Thalidomide starved them.
In 1998, the FDA approved thalidomide for a specific leprosy complication called erythema nodosum leprosum. In 2006, it got a second approval - for treating multiple myeloma, a deadly blood cancer. Clinical trials showed patients lived longer. Progression-free survival jumped from 23% to 42% over three years. But there was a catch: up to 60% of patients stopped taking it because of nerve damage - numbness, tingling, pain in hands and feet. Still, for many, it was a lifeline.
And then, in 2018 - exactly 60 years after the first affected baby was born - scientists finally figured out how it worked. Thalidomide binds to a protein called cereblon. In embryos, this disrupts the signaling needed to form limbs. In cancer cells, it triggers the destruction of proteins that help tumors survive. One molecule. Two outcomes. One tragedy. One breakthrough.
How It’s Used Today - And Who Can’t Take It
Today, thalidomide is sold under strict controls. In the U.S., it’s only available through the System for Thalidomide Education and Prescribing Safety (STEPS). This program requires:
- Women of childbearing potential must use two forms of birth control
- Monthly pregnancy tests
- Signed agreements acknowledging the risks
- No sharing or selling the drug
Men taking thalidomide must also use condoms - the drug can be present in semen. Even a drop can cause damage. The FDA calls thalidomide “one of the most potent human teratogens known.” And it’s right.
Still, it’s used. Thousands of people with multiple myeloma, leprosy complications, and certain autoimmune diseases take it. Annual global sales hit $300 million by 2020. It’s not a cure. But for some, it’s the only thing that works.
What We Still Don’t Know
Why did so many doctors ignore the early warnings? In 1960, patients started reporting numbness in their hands - a sign of nerve damage. The manufacturer added a warning to the packaging. But no one connected it to pregnancy. Why? Because the science of fetal development was primitive. We didn’t know how early organ formation happened. We didn’t understand pharmacokinetics in pregnancy. We assumed what was safe for adults was safe for babies.
Today, we know better. But we still have gaps. We don’t have good data on how thousands of medications affect developing fetuses. Most drugs aren’t tested on pregnant women - ethically, they shouldn’t be. So we rely on animal studies and post-market reports. And those are slow. And incomplete.
Thalidomide taught us that absence of evidence isn’t evidence of absence. Just because a drug hasn’t been proven dangerous doesn’t mean it’s safe. Especially in pregnancy.
Lessons That Still Matter
Thalidomide isn’t just a historical footnote. It’s a living lesson.
- Never assume safety. Just because a drug is widely used doesn’t mean it’s safe for everyone.
- Ask the right questions. What happens to the fetus? What happens to the baby? What happens to the child years later?
- Listen to the outliers. The first signs of harm often come from a few strange cases - not mass data.
- Regulation saves lives. Kelsey’s refusal wasn’t bureaucracy - it was foresight.
- Science evolves. Thalidomide went from poison to medicine. That’s not a contradiction - it’s a reminder that drugs are tools. Their use depends on context, control, and knowledge.
Every time a pregnant woman fills a prescription - for nausea, anxiety, pain, or infection - she’s relying on a system shaped by that tragedy. The testing. The warnings. The monitoring. All of it came from those 10,000+ babies who never got a chance.
Today, the Science Museum in London has a permanent exhibit on thalidomide. Medical students around the world study it. Pharmacists are trained on its risks. And every time a woman is told, “Don’t take this during pregnancy,” someone remembers the price of forgetting.



Lou Suito
February 26, 2026 AT 12:39lela izzani
February 26, 2026 AT 23:13Christopher Wiedenhaupt
February 27, 2026 AT 02:30John Smith
February 28, 2026 AT 19:41Shalini Gautam
March 2, 2026 AT 05:47Natanya Green
March 2, 2026 AT 15:34Steven Pam
March 4, 2026 AT 12:39Timothy Haroutunian
March 5, 2026 AT 16:45Erin Pinheiro
March 5, 2026 AT 21:46Michael FItzpatrick
March 7, 2026 AT 21:12Brandice Valentino
March 8, 2026 AT 04:40Larry Zerpa
March 10, 2026 AT 01:02Gwen Vincent
March 11, 2026 AT 10:13Nandini Wagh
March 11, 2026 AT 15:02Holley T
March 13, 2026 AT 02:58